Farhin Patel
Patel Farhin Heading link

Basic Information about Student (Small Background introduction)
Year: Senior
Area of Research: Opthalmology
Contact Information: fpatel29@uic.edu
Blog Heading link
-
Week 1
Picture

picture
blog
Dr. Jain from Lions of Illinois Eye Research Institute specializes in Dry Eye Disease. On a normal clinic day, each of the team members got to see about 10-15 patients. Dr. Jain always had two assistants present whenever he saw a patient. We saw tear collection, Oculus keratograph imaging, Lipiview imagaing, osmolarity test, pressure check, tear collection and eye staining.
Good Designs: Two waiting rooms which prevented overcrowding of the waiting room and faster flow of patients, presence of a pharmacy in the facility, presence of two assistants made the tear collection process more efficient, charging outlets in the waiting room kept the patients occupied on their phones while waiting, two examination rooms with larger length provided perfect distance for vision test.
Bad Design: Tear collection process required presence of two assistants which in small rooms created crowding, some imaging devices were only found in one examination room so if a patient needed a Lipiview imaging or Keratograph, the patient had to be moved. Photography equipment were only in one examination room that is why in all the other rooms the doctor could not take reference images to check for progress.
-
Tear Collection Process
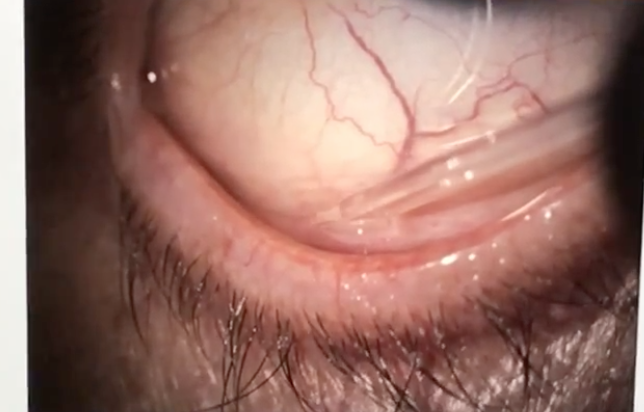
Tear collection is usually done in the presence of a doctor, patient and two assistants.
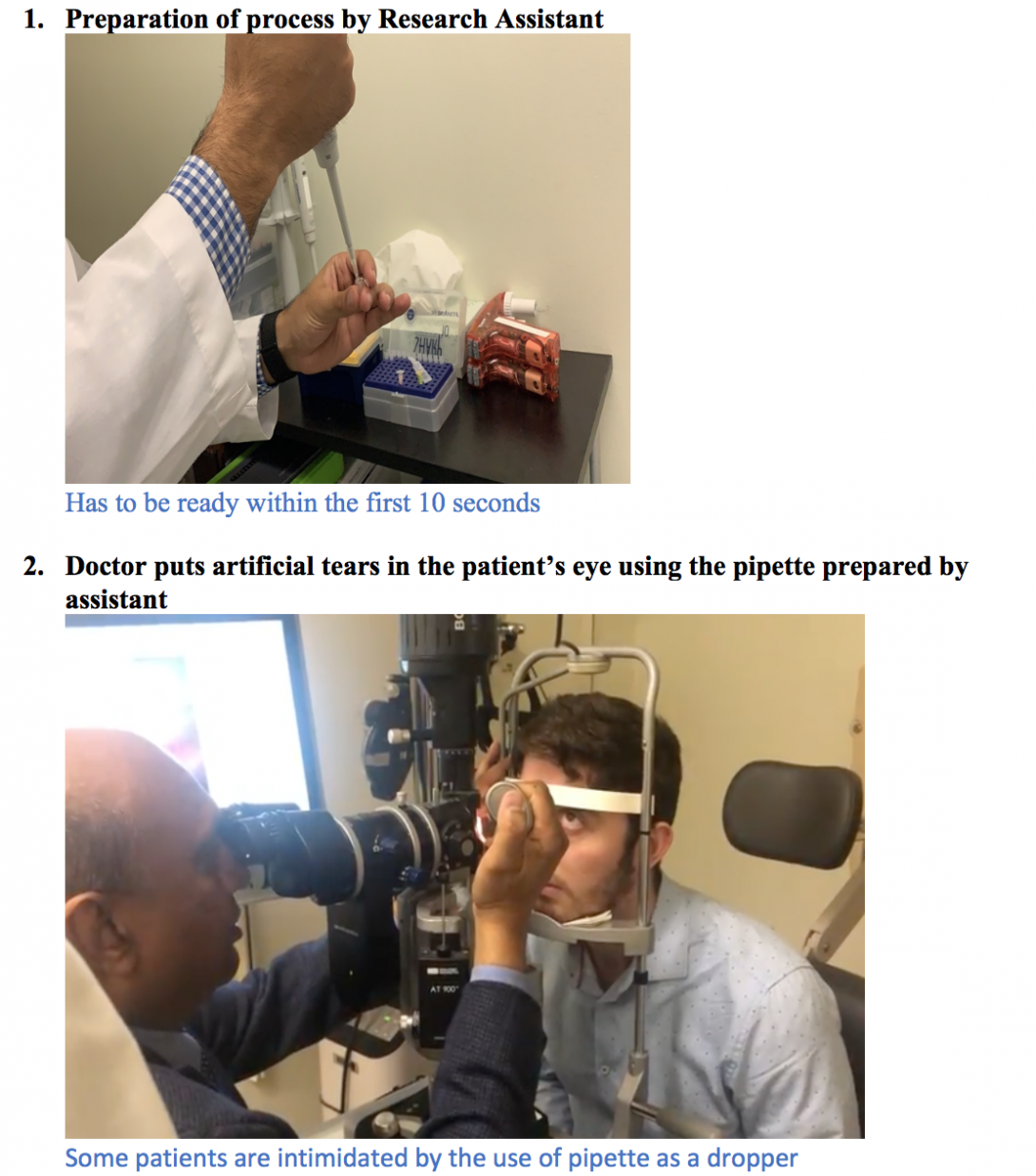
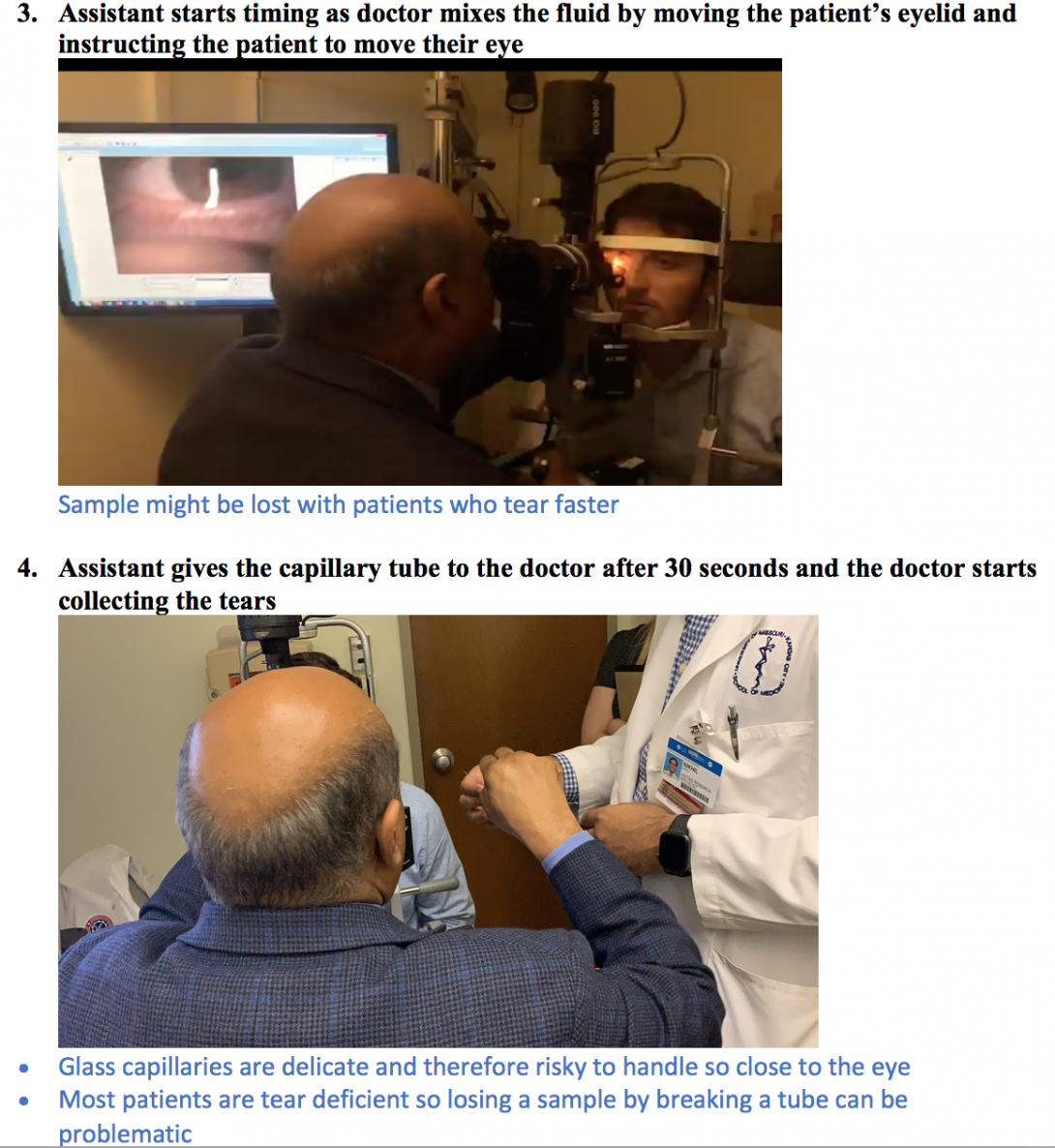
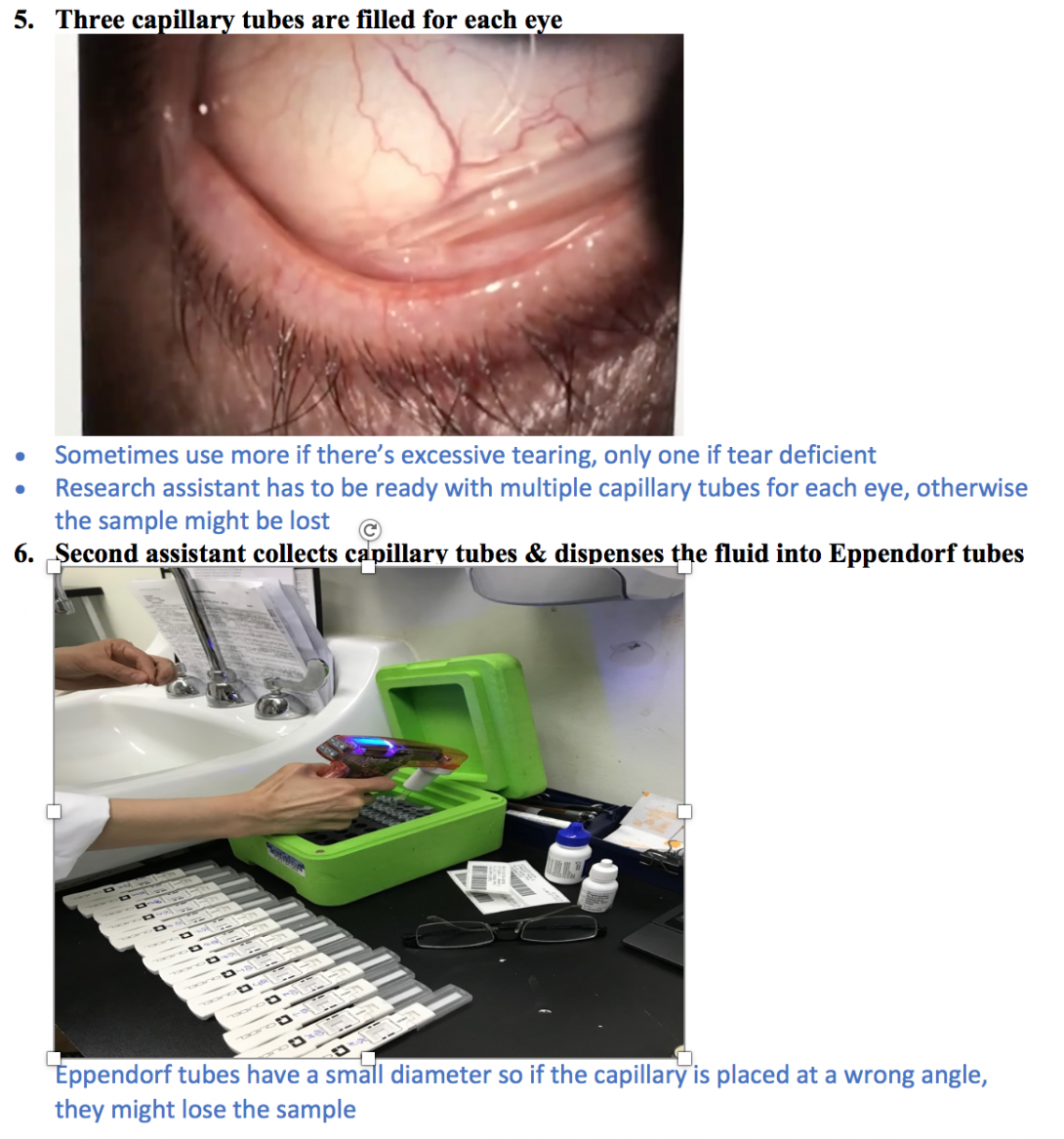

-
Week 3
This week in opthalmology, my team and I worked on the needs statement and evaluated various problems. Dr. Jain performed two processes, the tear collection and lissamine green staining with all the patients so we got a good insight of the process. We noticed problems with both processes. However, we chose to proceed with the tear collection because it is very demanding and risky process.
Need Statement:
- To make the tear collection accessible for more healthcare workers and safe for patients
- To modify the tear collection process to make it user friendly for more healthcare workers to use safely on patients
- To create a more user-friendly tear collection process that allows any healthcare professional with minimal training to collect patients’ tears safely
-
Week 4
Finalizing the needs statement and brainstorming laid out the way for design criteria and specifications. My team and I categorized the specifications into four sections named comfort, efficiency, safety and accessibility.
Comfort Criteria:
- The device should remain in the eye for less than 10 seconds at a time.
Our eyes tend to get irritated once something stays in it for a while. Therefore, removing the device from the eye in 10 seconds ensures that it does not irritate the eye. Hence, making it comfortable for the patient.
Efficiency Criteria:
- The entire process of tear collection should be done within a minute
- The device should collect minimum 50 µL of tear sample from each eye in a healthy patient (with no dry eye conditions)
The current process of tear collection which requires the presence of two assistants in addition to the ophthalmologist, takes about 2 minutes in total. We want the device to collect the sample from one eye at once instead of using multiple capillaries. This should cut down the time for the tear collection process.
Safety Criteria:
- The device should not cause injury to the eye
- Materials that touch the eye should be sanitary
- Materials which come in contact with tears should be disposable
Safety of the user and the person the device is used upon is of utmost importance so we want to make sure the device does not cause any abrasions or bruising to the surrounding tissues. In addition to that, we want to ensure that the device has a part that is disposable/ recyclable in order for the process to be free of contamination.
Accessibility Criteria:
- Healthcare professionals should be able to use it after one demonstration
- Should be handled by one person without additional materials (slit lamp)
One of the main reasons why tear collection for tear analysis is not done by many healthcare professionals is because of lack of resources. The current process requires the use of slit lamp which is not available to all healthcare professionals. Training is also another problem. The use of glass capillaries requires utmost stability and precision which requires a lot of training. We want our design to aid with that so that the healthcare professionals are able to use after one illustration is done.
-
Week 5
This week as each team member drew out a prototype on concept card, we realized that it was the best way to communicate it to my team members and others. We were advised to talk to our mentor and separate the good and the not so good features of the prototype. We were debating over using a motorized vs. mechanical design. After our meeting with Dr. Jain we concluded that motorized design was the better choice to make. We eliminated some features as well as it was not of much benefit as adding them was leading to a complicated design.
Our final need statement, “To create a more efficient tear collection process, increasing accessibility, while maintaining a safe and comfortable experience for patients,” and the design criteria were very helpful in refining our concept.