Ravi Tyagi
Ravi Tyagi Heading link

Basic Information about Student:
Ravi was raised in Naperville, IL and graduated from Saint Louis University in 2018 with a B.S. in Biomedical Engineering. His research dealt primarily with tissue engineering, regenerative medicine, and wound healing. His specific interests included the use of electrospinning for burn wound and pressure ulcer applications, and fabrication of 3D printed cryogel scaffolds for treatment of volumetric muscle loss. His hobbies include swimming, badminton, and hiking. He hopes to use his background in engineering and experience with IMED and CIP to make healthcare more efficient, affordable, and accessible.
Year: M2
Area of Research: Urology
Blog Heading link
-
"Good" and "Bad" Engineering
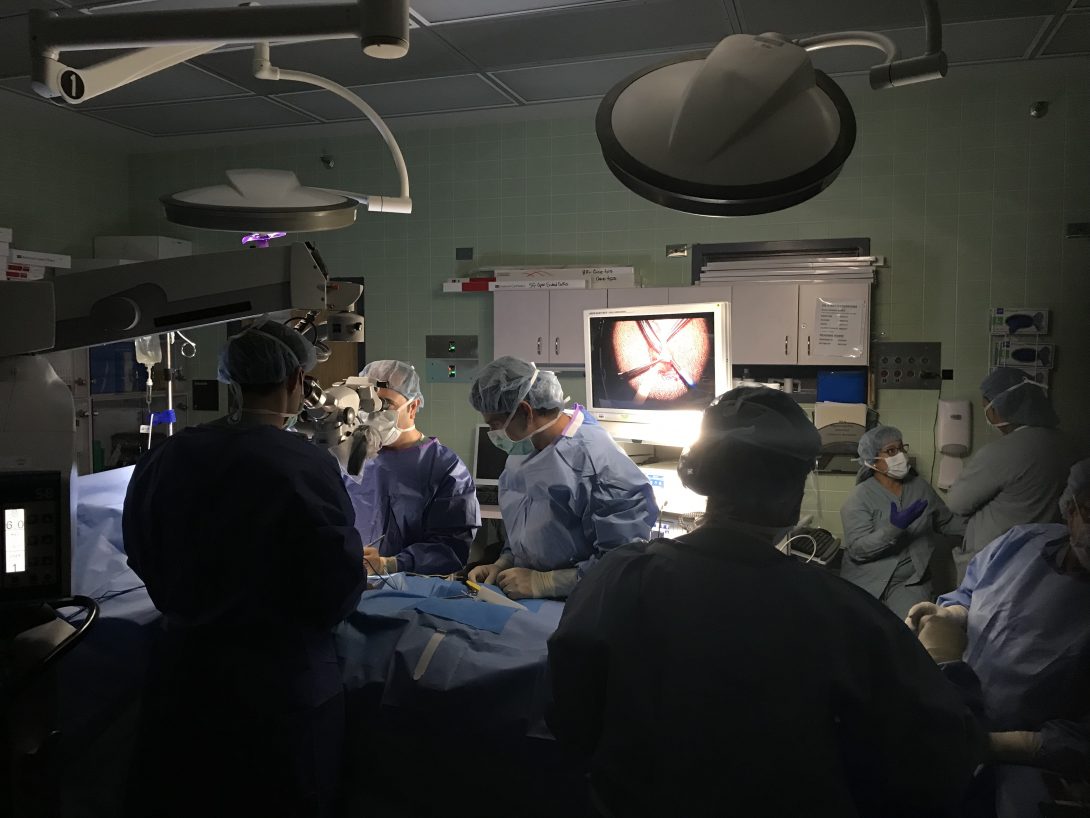
This week we had the opportunity to observe in both the clinic and in the OR. One of my favorite cases we observed this week was the varicocelectomy. There were a number of interesting technologies utilized including an ultrasound transducer used to identify the location of blood vessels. The transducer was an essential part of the procedure because without it identifying the vessels from the fascia and other tissue of the inguinal canal would prove challenging. The transducer allowed the surgeons to identify and ligate the veins in the region while also allowing them to preserve the testicular artery.
The device uses the doppler effect to identify blood flow to a region. What makes this device unique is that instead of providing another visual stimulus for the surgeons to interpret, it provides an auditory stimulus. The surgeons already have so much to focus on during the procedure, so using the transducer provided a novel stimulus to avoid sensory overload.
I was initially skeptical as to how beneficial clinic would be towards finding needs, but I was surprised by how quickly I identified areas to improve flow in the clinic. One device that could be improved is the probe for the urogram. For one, the probe placement is pretty invasive and uncomfortable for the patient. Moreover, even slight misplacement of the probe could render the 30 minute ordeal of setting up the device meaningless and make the patient’s discomfort go in vain.
-
Storyboard
One of the most common procedures performed in urology is cystoscopy. Cystoscopy is performed to visualize the bladder and urethra using a camera. While other imaging modalities like X-ray, CT, ultrasound, and MRI have the advantage of being non-invasive, cystoscopy can sometimes be the most definitive way to understand the pathology.
The procedure can be performed in the clinic or in the OR, but the steps are similar. First the patient is consented to the procedure, then they are brought into the procedure room. The area around the urethra is sanitized with iodine and local anesthetic is injected into the area. A catheter is inserted into the urethra to expand the urinary tract with water. The cystoscope is inserted and used to view urinary tract. The physician will examine the video footage of the tract to identify pathology or to orient themselves in order to perform a procedure. Finally, the water is drained from the tract and the scope is removed.
One of the pain points that we recognized through this procedure was the difficulty in coordinating all the moving parts. For example, the physician would often struggle to position the scope, the phallus, and a probe without another person being there to assist with the procedure.
-
Needs Finding
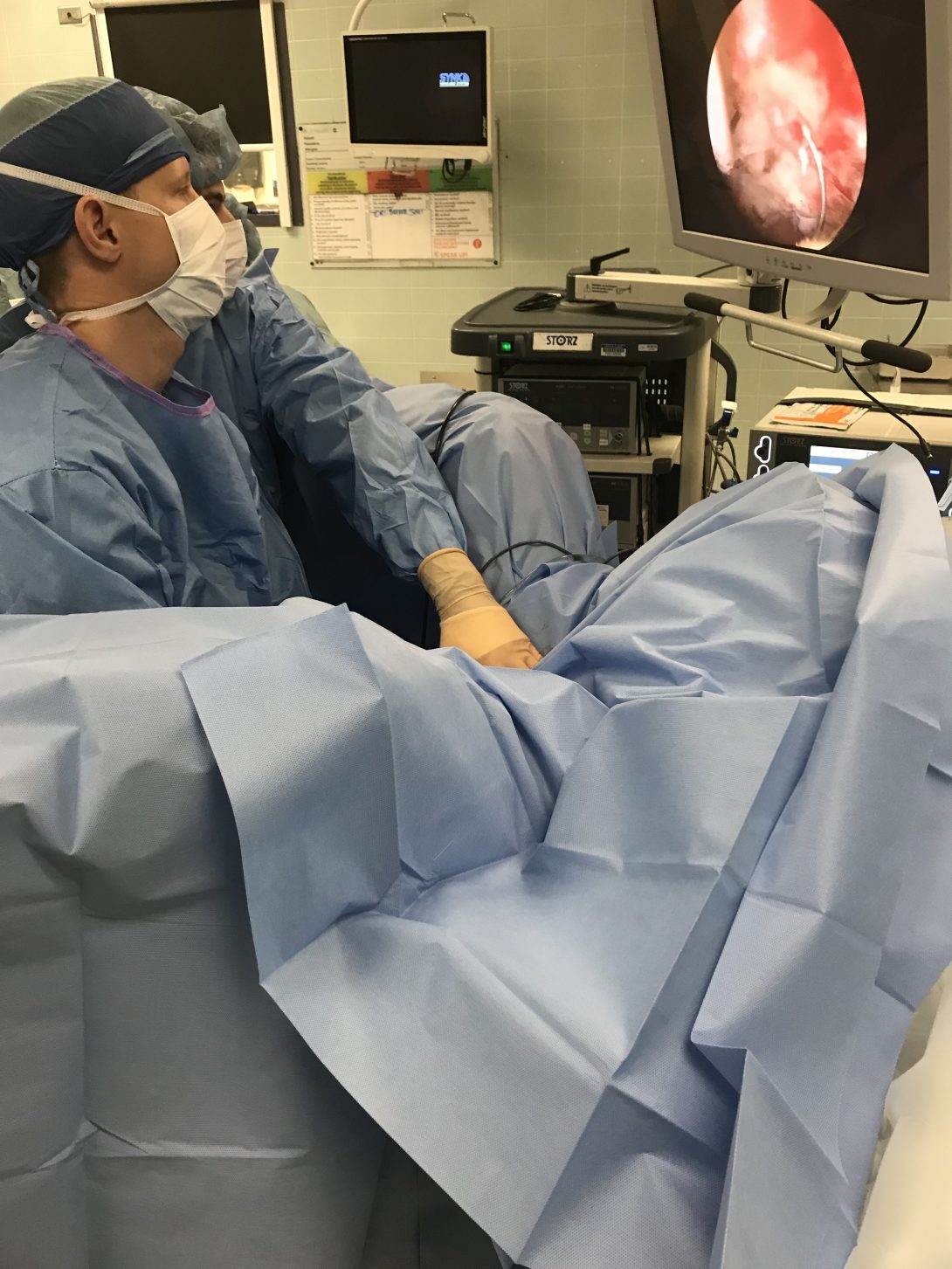
This week our objective was to begin thinking about framing some of the observations that we made into need statements. For the past couple weeks, I’ve noticed that surgeons are consistently limited in their dexterity during cystoscopy. The procedure requires the use of three hands at times: one to position the camera, one to position the anatomy, and one to navigate other tools into the urethra. After talking to the surgeons, it seems like this problem is most troubling at the beginning of any procedure requiring cystoscopy: especially those performed on males since it requires positioning of the phallus. That being said, here is the need statement we came up for this week.
Need Statement: A way to position the cystoscope to increase physician dexterity during procedures requiring cystoscopy.
-
Constraints and Specifications
This week our goal was to narrow down the list of potential improvements we would like to make and choose one to focus on for the remainder of the program. After interviewing nurses, residents, and attendings, one idea that stands out is a redesign of the prostate biopsy gun. The current gun collects one sample at a time and requires the physician to reinsert the ultrasound probe into the rectum 12 times to obtain the specimen. Additionally, the gun makes a startling noise every time the sample is acquired which invariably startles the patient. Our goal is to redesign the gun to make it more convenient for the physician and comfortable for the patient
Some initial constraints we developed include:
- The device shall be used for prostate biopsy.
- The device should be used in clinic/in the OR for patients with a PSA more than 4.o
- The device shall collect one biopsy core at a time.
- Each collection should take no more than a minute.
- The device should be operable by one physician.
- The device shall fit within a 5000 cc volume.
- The device shall be spring-loaded but may contain an electrical power source in the form of a battery
- The electrical source should last for at least 2 hours
- The device shall be plastic and needles will be metal.
- The device will be no louder than 50 dB.
-
Concept Cards
One of the objects of this week was to narrow down on the idea for our project and start conceptualizing potential solutions. We quickly discovered that it was far too easy to get lost in the weeds and lose sight of the bigger pictures. For the remainder of the class, we chose to focus on the prostate biopsy gun. Specifically, we wanted to find ways to make the biopsy experience more comfortable for the patient and more intuitive for the physician.
We had a number of “solutions” in mind prior to coming into this week. Perhaps we could create a “semi-automatic biopsy gun” to speed up the process? Perhaps we could incorporate some sort of “silencer” to lessen the patient’s fears? We quickly realized that before we pursued any of these ideas, it would be important to consult our stakeholders.
Fortunately for us, we were able to present our ideas directly to our stakeholders. The three components we wanted to focus on for the project were to:
- Design a quieter firing mechanism.
- Design a more efficient cocking mechanism.
- Design a faster way to load samples into the collection vial.
We already had ideas for each of these three needs, but after talking to our stakeholder, we realized that we might have bit off more than we could chew. Using the concept cards, he suggested that we focus on one of the three needs we identified: the sound. So for the rest of the week we experimented with ways we could reduce the sound of the biopsy gun.